|
The features extracted by the histogram-oriented gradient (HOG) and convolutional neural network (CNN) from X-ray images were fused to develop the classification model through training by CNN (VGGNet). This research has proposed a machine vision approach to detect COVID-19 from the chest X-ray images. Chest X-ray images are primarily used for the diagnosis of this disease. Earlier detection of the COVID-19 through accurate diagnosis, particularly for the cases with no obvious symptoms, may decrease the patient’s death rate. In December 2019, the coronavirus spread rapidly around the world, thought to be originated from Wuhan in China and is responsible for a large number of deaths. Watch the related VIDEO: How to Image COVID-19 and Radiological Presentations of the Virus - Interview with Margarita Revzin, M.D.Currently, COVID-19 is considered to be the most dangerous and deadly disease for the human body caused by the novel coronavirus. Image submissions with caption information can be sent to. New images will be added throughout 2022, as the world continues to face the struggles of the Omicron variant. The images were collected from physicians, study authors, universities and hospitals, the National Institutes of Health (NIH), the Radiological Society of North America ( RSNA), the American College of Radiology (ACR), Centers for Disease Control and Prevention (CDC) and radiology technology vendors.ĬLICK on the images below to show the caption information. CT and mobile X-ray systems are also used as front-line imaging systems for COVID-positive or suspected COVID patients. Ultrasound, especially hand-held ultrasound imaging devices, have become a primary imaging modality for novel coronavirus because of the ease to bag the device and sterilize it after use. The radiology images show examples of typical COVID pneumonia in the lungs and the numerous complications the virus causes in the body in multiple organs, including the brain, kidneys, heart, abdomen and vascular system. This photo gallery shows the variety of radiological presentations of COVID-19 (SARS-CoV-2) in medical imaging, including computed tomography (CT), radiograph X-rays, ultrasound, echocardiograms and magnetic resonance imaging (MRI). Image courtesy of the Radiological Society of North America At the 2-month follow-up, residual GGO and small subpleural microcystic changes (thick arrow) were noticed (H), which persisted up to 1 year after onset (I). Chest CT of a 79-year-old man (lower row, G-I) displayed bilateral consolidations and small areas of GGO while admitted to the ICU (G). However, subtle reticulation and GGO could still be detected (F). At the 1-year follow-up, further improvement was noticed. At the 2-month follow-up, a substantial improvement of OP pattern was noted with GGO and subpleural reticulation including arcade-like sign (arrowhead) in the left lower lobe (E). Chest CT of a 68-year-old-man (middle row, D-F) demonstrated patchy bilateral consolidations, a subpleural arcade-like sign and pleural effusions during active infection (D). These subpleural reticulations (arrow) persisted up to one year after onset (C). At the 2-month follow-up almost complete resolution of GGO with residual subpleural reticulation in the middle lobe was noted (B). Chest CT of a 44-year-old man (upper row, A-C) displayed extensive bilateral GGO and supleural reticulation during acute COVID-19 (A). Serial non-contrast axial chest CTs of three study participants with prior COVID-19 pneumonia. CT extent of pneumonia was scored as 2 (>25% involvement) and was classified as typical appearance of COVID-19 according to the RSNA chest CT classification system. ( H) Axial chest CT image obtained on the same day showing multifocal ground-glass opacities with a crazy-paving appearance in bilateral lungs. 
CXR extent of pneumonia was scored as 2 (>25% involvement). 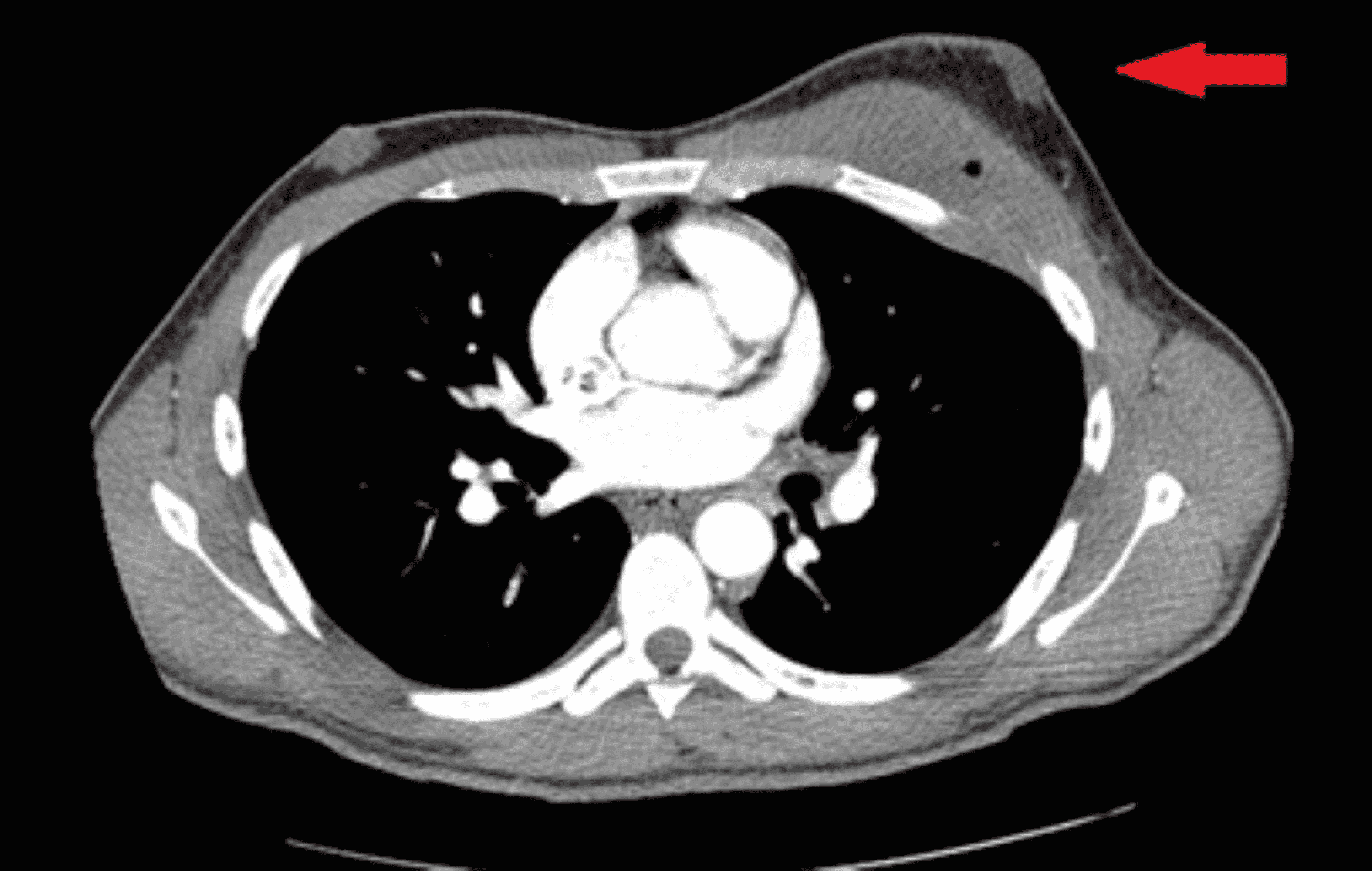
( G) CXR at admission showing patchy ground-glass opacities in both middle- to lower-lung zones. He required supplemental oxygen on admission and was admitted to intensive care unit one day later. The patient had a history of hypertension and diabetes. ( G and H) A 58-year-old male with no history of COVID-19 vaccination. CT extent of pneumonia was scored as 1 (1-25% involvement) and this case was classified as indeterminate appearance of COVID-19 according to the RSNA chest CT classification system. ( F) Axial chest CT image obtained on the same day showing unilateral ground-glass opacity with a nonrounded morphology and non-peripheral distribution in the left upper lobe (arrows). CXR extent of pneumonia was scored as 0 (no evidence of pneumonia). ( E) CXR obtained at admission showing no abnormal opacification in either lung zone. The patient had no history of comorbidity. ( E and F) A 36-year-old male with no history of vaccination for COVID- 19. 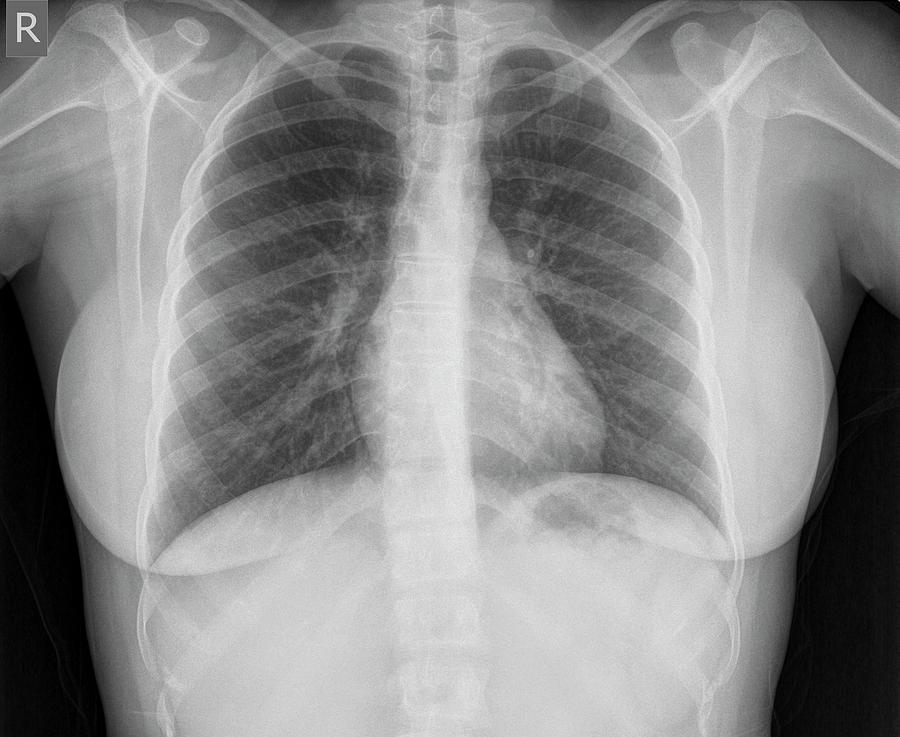
Representative cases showing pneumonia extents and patterns on chest X-ray (CXRs) and CT images.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
